The Star Legacy Foundation is frequently contacted by couples that have been told their child was stillborn due to an umbilical cord accident. Yet, many obstetricians will also say that babies are born all the time with a nucal cord (cord around the neck) and dismiss that as a cause of a stillbirth. Cord issues aren’t just limited to nucal cords. Simple compression, cord wraps around other body parts, torsion (twisting to the point of coiling back upon itself like a telephone cord does when twisted too many times), and true knots are also known to cause stillbirth.

Many of the same callers ask us what we know about Dr. Jason Collins and his work involving cord accidents. Dr. Collins, an obstetrician, has dedicated his career to stillbirth research and umbilical cord accidents specifically. The following is a brief summary of a presentation he recently gave at the Stillbirth Summit (October 4-6, 2011 in Minneapolis, MN, USA) which is a very high level overview of his research and conclusions.
================================================================================================================
The presence of umbilical cord issues have been well documented in published literature since the 1700s. Yet, this remains an area of obstetrics that is greatly understudied and ignored. The umbilical cord, the insertion site, the placenta, and the baby should be evaluated and characterized with every pregnancy. With advancing imaging technology, it is becoming even easier to identify areas of concern on ultrasound as early as 10 weeks of gestation.

Umbilical cord torsion occurs when the number of twists exceeds the ability of the cord to withstand the force generated. The cord compression generated causes fetal hypoxia (lack of oxygen). On placental exam, chorioangiosis (cellular changes) can be identified as a result of ischemia (restriction) due to cord compression. The length of the cord determines the amount of twisting that is harmful. The human umbilical cord will tolerate one twist per 5cm of cord length. Twists exceeding this ratio are associated with torsion and fetal death. The length of the umbilical cord and the number of twists present should be identified and documented at every delivery. Identification of torsion prenatally allows for altered management of the pregnancy with a better chance of a positive outcome.
There are two types of nuchal cords: type A and type B. Type A is a wrap that can possibly be undone with movement or delivery of the baby. Type B is a hitch that is impossible for the baby to release. If a type B loop around the neck, ankle, or other body part is pushed off the body, a true knot is formed.
With umbilical cord issues, the factor that determines the risk is the amount of slack available. For this to be determined, the cord location, cord structure, placenta, placental position, cord length, insertion site, and position of the baby must all be evaluated and considered. Short cords have been associated with an increased risk of neurologic insults and long cords have been associated with an increased risk of fetal death.
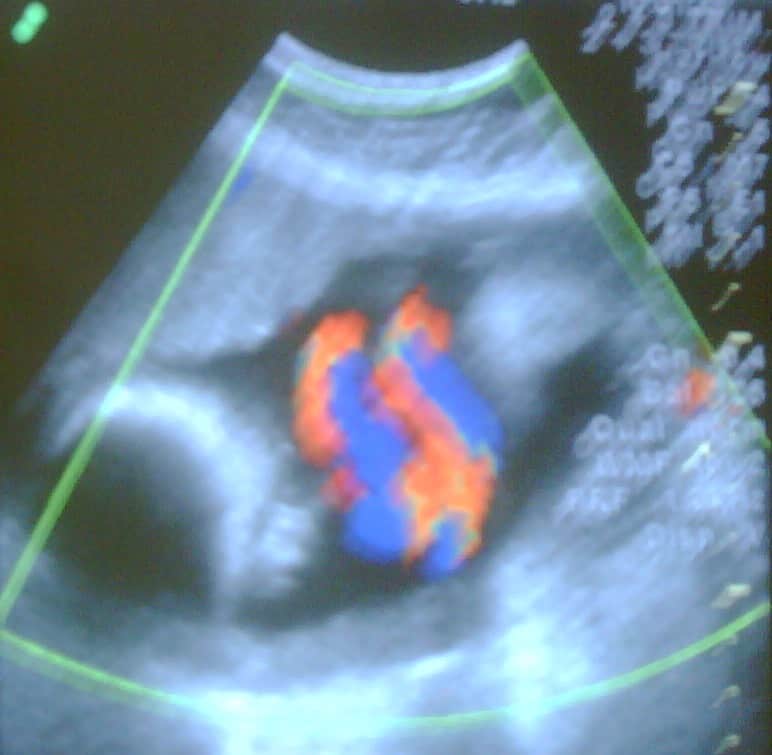
Work at the Pregnancy Institute has indicated that hyperactivity, hypoactivity, and hiccups may be clinical indicators of fetal distress. Women presenting with these symptoms should be evaluated for sources of cord compression. Fetal heart rate can provide information on this compression as well. Frequent decelerations, “W” signs, lambda signs, and spikes should be taken as indicators of fetal distress and managed accordingly. The exact amount of time that it takes for fetal chemistry to return to normal after cord compression has not been studied, but we estimate that more than three compressions in ten minutes would create increasing blood chemistry concerns and should be dealt with immediately.
Interviews at the Pregnancy Institute have also revealed that a vast number of fetal deaths occur during maternal sleep between the hours of midnight and 6am. Maternal low blood pressure may play a significant role in this finding as a reduction in blood pressure may alter the fetal response to underlying cord issues. Melatonin is produced during sleep and is known to affect the uterus. During these overnight hours, the melatonin produced stresses the uterus and the baby is challenged. Babies with cord compression may not tolerate this stressor.
Finally, work at the Pregnancy Institute has identified that umbilical cord accidents are not random or rare. Women who have had umbilical cord issues with previous pregnancies, have as much as a ten-fold increased risk of umbilical cord issues in future pregnancies. These women need additional monitoring for these concerns.
Management of umbilical cord issues is possible with proper diagnosis and fetal monitoring.
It is true that not all cord issues lead to stillbirth. However, it is also true that cord issues are a significant risk factor and cause many stillbirths. The evaluation of the umbilical cord and placenta should be included in a new standard of care for obstetrics in the 21st century.
==========================================================================================
About the author:
Lindsey Wimmer, a Pediatric Nurse Practitioner, is Mom to four children; Garrett who was stillborn in 2004, Grant, Bennett and Austyn. Lindsey and her husband Trent founded the Star Legacy Foundation shortly after Garrett’s birth. At that time they came to realize that the numbers of stillbirths in the US were staggering and that very little was being done to determine the causes or find prevention initiatives. Visit the Star Legacy Foundation to learn more.


38 Comments
Coming from an infectious means of stillbirth background, I found Dr. Collins presentation at the Stillbirth Summit to really be an eye-opener for me as to the scope of the stillbirth problem. Thank you for the summary and please post any updates as they are available.
Absolutely Marti – updates will be forth coming! Thanks for your comments. And I must say that likewise, I was greatly enlightened by the presentations provided by Group B Strep International. The Summit clearly highlighted how complex the problem of stillbirth is – and that any one risk factor may or may not singly cause a stillbirth but the odds increase exponentially when multiple risk factors are present and create “the perfect storm.”
My heart stopped when I read about the Double tight nucal cord, maternal sleep, babies passing away during midnight and 6am. It brought back every memory of the Loss of my daughter Lilly on Sept 14th 2004. She too had the tight nucal cord times 2. She was alive when I went to bed and I knew she passed away when I was sleeping. Thank you for you research. After 7 years, this I believe is my peace of mind an answer. She also hiccuped all the time. Her loss has changed my life forever. She is always missed and our family will never be whole without her.
The topic is awesome
My brother suggested I might like this website. He was entirely right.
This post truly made my day. You can not imagine simply how much time I had spent for
this info! Thanks!
Why aren’t OBs aware of this my daughter just had a angel baby because no one was aware of this. I found out by googling. this needs to be brought to attention before a mother is having to bury her newborn. There is nothing that compares to watching your daughter cry as she rocks her dead baby. This has happened to two families in three months in a town of two thousand people. All mothers need to be monitored All the time not just high risk. This was my daughters first. She had low bp, baby had hiccups all the time, and his heart rate had decreased. They said it was dehydration so they gave her fluids sent her home. he was gone with in 24 hr. February 14 2013 7:10 pm our Angel baby was born. We need awareness! Both our Braxtyn and Ruger (nov 12,12) would be in their families arms not in a cemetery. Caskets that size should not even be needed. I am putting all I can on fb but these should be red flags for all obgyns and ERs
Families should not have to go thru this all the signs were there, but no one knew the signs!!! We need to stop this in all the technology this should be a thing of the past!!
RaeAnn,
I am so very sorry about your loss. You are so right about so many things – that no mother should have to witness her own baby rocking her dead baby; that all pregnancies should be considered high risk with the best monitoring and prenatal care available. These things are precisely why the Star Legacy Foundation was started – in an effort to encourage stillbirth awareness, research and prevention strategies. Please visit our website at http://www.starlegacyfoundation.org to learn more about our efforts.
Please call upon us if there is anything we can do to support you and your family.
I voiced my concerns in tears with my nurse over the phone and was basically told “you have an appt coming up Im sure everything is fine… i felt something was going terribly wrong in my gut yet I was dismissed. I went for an OB appt 1 week later and delivered my son at 17 1/2 weeks due to “a cord incident” the next day. I was happy to find this site and discussion as well. I feel deeply for your loss.
Do you guys have any research on coiled index with the cord? I just lost my baby last Tuesday, June 25th at 22 weeks and based on the pathology report on my placenta, my cord was over coiled and there was also a clot as a result. I can’t find any good solid research on this and if it is something that might happen again. I am desperate for help.
The Pregnancy Institute has done work on hypercoiling of the umbilical cord, but otherwise, there is very little research. What we do know is that it can reduce the blood flow through portions of the cord and is also easier for the cord to ‘kink’. We hear stories from women who have had repeat cord issues, but there is not sufficient research into how much this occurs or how or why. Many of these issues can be identified via ultrasound and then managed based on how the baby is doing, etc.
Hi. I had a baby born still in October 2005. It’s absolutely absurd that doctors do not routinely warn their patients about the risk factors of stillbirth or check the cord with an ultrasould. I had low blood pressure, and a doctor joked with me, “No wonder you’re tired. You’re almost dead.” My BP was sometimes 60/40 while I was pregnant. Two pregnancies went fine. Then I lost Savannah. She was hiccuping in my OB/gyn’s office the morning before she died, and the doctor joked that it was like she was knocking to get out. DUH! Those hiccups are not a joke. The next day, she was not hiccuping. We went for an ultrasound, and the US tech pointed out that what should have been lighting up like a Christmas tree was not. She had no blood flow. I pray that doctors will open their eyes and protect babies and their families from this horror.
My sweet angel was born sleeping due to a knot in his umbilical cord. I felt a decrease in fetal movement and went in later that night and was told baby had no heartbeat. I was nearly 39 weeks when I heard the news, I was devastated. From what I read above my future pregnancies have an increased risk of same problem? I dont think i could go through that again. How many studies are that statistic? – Worried sick
Dear Andrea; In 2001 my daughter lost her baby boy at 40 weeks pregnant due to a cord accident. Devastating. Ten years later she gave birth to a healthy baby girl and this year a baby boy. She is proof that it is possible to go on to have more children. I really hope this gives you faith to try again, if that’s your wish <3
I am so sorry, Andrea. It is true that statistics show women who have had a previous poor pregnancy outcome (includes premature birth, stillbirth, neonatal loss, etc) have a higher risk of a poor outcome in future pregnancies. What the actual numbers are vary from study to study and differ depending on what the cause of death was, or if a cause is known. Many times, the reason for the increased risk is not explainable. This is the main reason why most pregnancies after a loss are monitored as ‘high-risk’ with a different protocol for care from ‘routine’ pregnancies.
Hi, I’m so happy to finally see an article that makes sense to me. I just gave birth to a stillborn baby boy at 28 weeks and had no answers except he had the cord wrapped twice around his neck. He was my 3rd and sadly due to complications from the csection my last. No one, until I read this article had been able to give me feedback, I too had low BP, and he had hiccups the day it happened and decreased movement and like most it’s interesting he stopped moving between 12-6 a.m..How come Drs. are not made more aware of this, I called my OBGYN and was informed to come in the following day for my symptoms were not uncommon . I knew something was wrong, maybe if my cord had been monitored more in the ultrasound my angel would be with us now. This info needs to get out there and that way many future losses prevented.
Still grieving Anne.
My son was born on Dec 18th with a true double knot in his umbilical cord by csection. His estimated weight by ultrasound 2 months prior was 8 1/2 lbs but was born at 6lb 6oz at 39 weeks. god blessed us and he survived but now I am worried about if there are long term affects due to the knots. Any info on this would be greatly appreciated.
Hi Lillie – Thank you for sharing your story. You are exactly right that these events during pregnancy can have effects we don’t immediately see. There are several studies looking at all types of interrupted blood flow during pregnancy. Ultimately – there isn’t a way to predict because it all depends on the severity and duration of the issue along with the timing of the pregnancy. However, there are also many studies that prove the amazing ability of a baby’s brain and neurologic system to overcome many challenges. In any case, early detection and treatment always provides the best opportunity for minimizing poor outcomes. Your awareness and vigilance is a great sign for your son! I would encourage you to provide age-appropriate toys that will stimulate his senses and promote neurological development. Talk to your pediatrician for specific suggestions. Be sure to mention any questions or concerns you have about your son’s development with your pediatrician. Congrats and I wish you the best!
My daughter and her husband had an angel baby 1-8-14. She measured at almost 21 weeks, but she was supposedly 29 weeks along in the pregnancy. She had concerns about her small belly size, but her OB did not seem concerned at her 24 week checkup. This was her first pregnancy. She was also diagnosed at the beginning of her second trimester with ulcerative colitis, which caused a lot of stomach issues which mimicked the feeling of the baby moving. When little Brynn was born, the cord was around her neck, which her doctor said could have been the cause of death. Her placenta is being tested for many things to see if there were other issues. We are hoping for the result of those tests in a few days. I am wondering what the normal length of the umbilical cord is at 21 weeks gestation due to the fact that my sister lost her first baby due to an unusually long umbilical cord. Is this type of thing hereditary in any way? Just wondering.
According to Dr. Jason Collins of The Pregnancy Institute, the baby’s cord should be the length of the baby after 12 weeks of gestation. There is some speculation that there may be a hereditary or familial component to many cord issues, but it just hasn’t been studied well enough to say for sure. I hope you will be given answers for your loss.
I appreciate the reply.
My daughter just lost her baby girl at 33 weeks. She has turner syndrome had ivf with sucess all was fine till her blood pressure went up dangerouly high she saw her cardiolist that afternoon he sent her right through emergency. They kept her and she knew something was wrong. She was scheduled for a csection in March. She wanted them to do the csection and take the baby out but they didnt and she passed away. The nurses had checked at 2am there was a heartbeat then they shut the heart monitors off and at 4am they could not find a heartbeat. They scheduled her that morning after the baby was gone to do the csection we were told it had nothing to do with blood pressure but it was a cord injury the cord was wrapped around her ankle. But we feel 1 they should have taken and done a csection the night before becase she was high risk and 2 they should have never shut the heart monitors off. It would have alarmed them the baby’ss heart stopped. We feel this could have been prevented. Their reson they thought the baby better off inside mother as long as possible. I just wish they would have done a csection the night before. They had given the baby something for her lungs I think in case they took her but my daughter ate and she could have had trouble if they took and operated but my daughter and her husband are devasted they are going to try in a year the baby had hickups prior as well if anyone has had this happen especially having turner syndrome please let me know thanks
I lost my baby girl on 11-17-13 from an umbilical cord accident. My husband and I are desperate to try for another baby. I have had two c-sections, one 5 1/2 years ago and one in Nov. 2013. Does anyone know of a suggested wait time before trying again? I would love to hear what Dr. Collins suggests.
I’m so sorry for your loss. I’m not positive what Dr. Collins would say, but the literature and experts don’t provide a clear answer. I would say it depends mostly upon if a cause was identified for your daughter’s death. If so, your physician may suggest treatments, testing, genetic counseling, or other items to reduce or evaluate any future risks. The second major factor would be when you feel emotionally ready to enter another pregnancy. Of course, pregnancies after loss are always stressful, but some people feel better ready to handle that anxiety after more time than others. Again, research says various things about the timing, but I believe it is very individual. Finally, I would suggest having a meeting with your OB to discuss any questions or concerns you have including what the plan is for your next pregnancy. Many parents and many OBs have different ideas about what should be done the same or differently – and it is easiest to have this discussion and create a general plan before you are pregnant (or very far along into the pregnancy). If you and your OB do not agree on how the next pregnancy should be handled, it is acceptable to interview other providers until you find one that meets all of your physical and emotional needs.
On Nov. 10th it will be 27 years that the cord was wrapped around my baby boy’s neck, causing a stillbirth. When my daughter was born 18 months later, and induced 2 weeks early due to my previous pregnancy history, she was born with the cord wrapped around her neck, and the cord was cut before she was completely delivered. This tragedy would have happened again if not for her early delivery. So, what do you say to that???????
My daughter’s baby girl was stillborn just short of 38 weeks the end of May 2014. They told us it was a cord accident. I have spent the last nine months researching the subject and still don’t have the answers I have been desperately looking for. She had an ultrasound at her 37 week check-up and was told everything was fine. The baby’s respiration was a little slow and when my daughter asked if there was something wrong she was told no. The baby was in a posterior position so I can only assume that the cord was not visible. A few days later the doctors could not get a heartbeat and my daughter was induced and delivered the baby 1 1/2 days later. After reading the article above I realized that my daughter’s BP had seemed low during her pregnancy but she was never told that this could be a problem. Should her low BP and the baby’s respiration at 37 weeks sent up a flag?
My daughter is pregnant now and due the middle of July. Everything seems to be going well and we are all anxious and optimistic that we will meet our new granddaughter in a few months. Is there anything that she or her doctors should be doing to insure a favorable outcome. I have read Dr. Collins articles on the foundation website and have just downloaded his book to my tablet and will start reading it tonight.
My daughter is the most loving and caring young woman I know and to lose her first child to such a tragic accident seems so unfair. Unborn babies are having surgery while in their mother’s wombs with success, so why are so many babies dying from “cord accidents”.
I worked for over 25 years on Clinical trial databases and want to know why there is not more research being done to find a reason why these babies are dying.
What can we do to help?
So sorry for your loss, but happy at the upcoming new baby. I lost my baby 5 days before my due date, a boy, with the same cord wrapped around his neck. That happened November 10, 1987. On July 26, 1989, we had a beautiful baby girl, and now she is almost 26! I know the waiting is a very stressful time, but you have to believe that this will be a good outcome, with a wonderful, healthy baby to show for all the worry. Time does help heal, but you will never forget your little lost angel. All good wishes.
Thank you so much for your comment. Your well wishes were appreciated and your optimism was welcome. Our daughter gave birth to a beautiful 7 lb. 1 oz. baby girl on June 25th. She is just perfect and we are truly blessed.
Our daughter’s doctors really stepped up her care at 32 weeks with weekly ultrasounds and bi-weekly visits. They induced her early and the baby was born at 37 weeks.
Hi.joy iwas pregnant 37weeks but sad to say may baby die because of cord accident, i dont have any idea about the cord accident. Because my baby is healthy .i dont know the true fidings about his cord was accidentaly cut inside.do you think it can happened again if i get pregnant
unfortunely, i lost my baby girl in 7/11/2015. the autopsy, and my placenta exams doesnt gave me the reason for her dead. the only strange thing was that the cord was like a phone cable, and only had 37 cm.
I am doing a lot of exams, including ADN exams to find an answer for her dead!!
really hope this not happen to me again…
I guess i’m just so curious as to WHY women that have had a cord accident have a greater chance of the same outcome again? Is there research that shows why that is the case?
We lost our firstborn, a son in May of 2015 to a cord accident at 33 weeks, and are now 26 weeks along with our rainbow, a little girl. I started weekly appointments with a biophysical profile sono done at each appointment at 24 weeks. Everything has been good so far, but I just can’t help but fear. In my pregnancy with my son, he was so active. It was classified as a perfect pregnancy – but we only had 2 sonograms with him, one at 8 weeks, one at 20 weeks. To my knowledge, my blood pressure was never an issue, I think I felt him have the hiccups only one time. The 12 pm – 6 am strikes me most because I went to bed with him kicking me to sleep, woke up and didn’t feel him, but usually he started going after I had breakfast and I had some cereal quickly, then was in a hurry to get to my 32 week appointment that morning. It didn’t occur to me that I hadn’t felt him yet by the time I got there, I had noticed some decreased movement but was told by every resource that by this point, he was running out of room so movements were becoming limited. I was completely blindsighted when he didn’t have a heartbeat at that appointment. Once I was admitted to labor and delivery and they were about to induce labor, they did another sonogram to check placenta, fluid and cord. They said based on that sono, they thought it could be cord, but wouldn’t know until he delivered. As soon as he came, my doctor confirmed that it was the cord – but I didn’t know WHAT exactly made it a cord accident. I didn’t know there were varying types. I haven’t been able to bring myself to ask her that question now in this subsequent pregnancy, but I’m sure it’ll be blurted out soon in an appointment. I find myself not wanting to go to that place of grief, fear and worry with others but then have moments where the unanswered questions consume me in private.
This time, I have a fetal doppler heart monitor at home. It is really just for reassurance, I hardly use it because I feel her kick so often but I’m glad I have it just in case I need to hear those beats. Our little girl had hiccups in 2 of the ultrasounds that we’ve had so far but they were earlier ones. The last 3 weeks of sonograms she has not had hiccups.
I appreciate you and for Dr. Collins’ research. I am so glad that the Pregnancy Institute exists.
Katie – I, too, wish we knew why there was a greater risk of this happening again. There are several theories and a few people studying it – but we don’t know. I am hopeful that additional studies and genomics work will give us some answers. Congratulations on this pregnancy and I wish you the very best. I know the anxiety that accompanies this pregnancy – so I also wish you peace and comfort! Thank you for sharing your story.
I went to the doctor 2 weeks prior to loosing my baby girl. I had a small slot of blood after going to the restroom went into the er thinking it was nothing serious went up to labor & delivery they found no heartbeat. My doctor said she couldn’t think of anything because she had just saw me 2 weeks ago. So I got induced around 3 am that morning & gave birth to a still born at 10:40 2/25/2020 her cord was wrapped around her neck twice.